A 72-year-old woman presents with increasing breathlessness over 3 days, orthopnoea, and paroxysmal nocturnal dyspnoea. PMH: Hypertension, atrial fibrillation. O/E: Appears distressed. Bilateral basal crackles and pitting ankle oedema present.
Observations & Investigations:
- HR: 110/min (Irregularly irregular)
- BP: 165/95 mmHg
- RR: 28/min
- SpO₂: 88% on room air
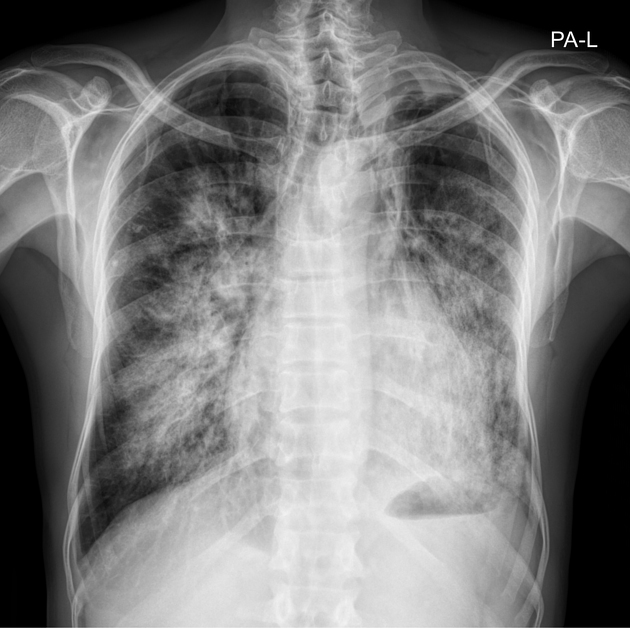
- CXR: Upper lobe venous diversion, cardiomegaly, and bilateral perihilar shadowing.
What is the MOST appropriate initial management?
Oxygen therapy, nebulised salbutamol, IV hydrocortisone, and oral prednisolone
Continuous positive airway pressure (CPAP), IV furosemide, and IV antibiotics
Oxygen therapy, IV furosemide 40-80mg, GTN infusion, and sit patient upright
Oxygen therapy, IV furosemide 40mg, and arrange urgent echocardiography
Non-invasive ventilation (BiPAP), IV morphine, and urgent cardiology referral