A 45-year-old man presents to the Emergency Department with a 12-hour history of a painful, swollen right leg. He has a history of type 2 diabetes mellitus and recently sustained a minor abrasion to his shin while gardening 3 days ago.
On examination:
- Temp 38.7°C, HR 125, BP 102/65, RR 24.
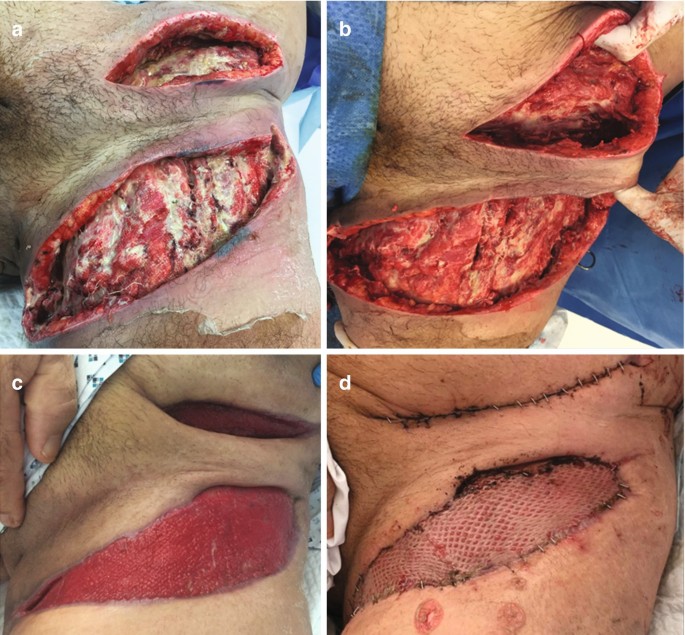
- His right lower leg is exquisitely tender, with crepitus palpable in the subcutaneous tissues. There are purple-grey patches and several bullae forming on the skin. A reference image demonstrating the required surgical management for this condition is provided.
Blood results show:
- WBC: 18.2 × 10⁹/L
- CRP: 285 mg/L
- Creatine kinase: 3,400 U/L
- Lactate: 3.8 mmol/L
What is the most appropriate immediate management for this patient?
A
IV flucloxacillin, arrange urgent surgical review within 6 hours
B
IV ceftriaxone and metronidazole, MRI before surgical intervention
C
IV co-amoxiclav, mark erythema, reassess in 4 hours
D
IV clindamycin and benzylpenicillin, emergency debridement
E
Give IV vancomycin, Doppler ultrasound to exclude DVT